
Volunteer led services
In addition to fundraising and delivering its own services, and supporting local initiatives and charities, over the past twenty-five years St John Scotland has developed four core volunteer-led core services, all aimed at saving lives. These services are Patient Transport, CPR Training, Public Access Defibrillators, and Community First Responders.
PATIENT TRANSPORT
Around 1997, Dr John Calvert, a St John Scotland volunteer, was instrumental in creating a Patient Transport Service to serve patients living in the Dumfries and Galloway Area. The service was operated by volunteers using their own cars to take people to and from their homes for the regular journey between Dumfries and Edinburgh for cancer treatment in Western General Hospital. Four years later, in 2001, the service’s capability was increased by buying a people carrier vehicle to complement the existing service. By 2007, the service had two dedicated people carriers funded by St John Scotland, driven by volunteers from both Stranraer and Dumfries. In addition, volunteers continued to use their own cars when necessary.
As well as same-day treatments, the service also provided transport to take patients to St John Home Cramond, which operated in conjunction with the Western General Oncology Department to provide accommodation for cancer patients from South-West Scotland who were undergoing longer radiotherapy or chemotherapy treatment sessions in Edinburgh. However, in 2007, the opening of a new unit at the Western General Hospital meant that the St John Home Cramond was no longer required for this service and it closed at the end of November that year. In 2009, Patient Transport in Dumfries and Galloway transported 490 people a total of 50,716 miles.
By 2006, St John Scotland Angus and Dundee Chair, Bill Spence, and his Area Committee had investigated the need for a Patient Transport Service for their area similar to the service running in Dumfries and Galloway. Having established that there was indeed a need for transport, the team started making preparations and turned their attention to recruiting volunteer drivers. The new service, which got underway on 1st May 2008, was initially geared to transporting up to four chemotherapy patients to and from Ninewells Hospital in Dundee, on five days a week. Drivers used their own cars and were reimbursed for their expenses. Requests for the service were made through the hospital. In addition, at the request of the Scottish Ambulance Service, transport was provided for people travelling to the Dialysis Unit in Arbroath and this increased the workload of the volunteer drivers immensely. A dedicated vehicle became necessary and was bought in 2009, though volunteer drivers continued to use their own cars and claim back expenses as required. The new vehicle was purchased thanks to a very kind legacy left by a local resident who wanted to support the service. During 2010, a total of 3,083 (2009: 2,100) patient trips covering 125,000 miles (2009: 55,100 miles) were undertaken by St John Scotland’s Angus and Dundee Patient Transport Service.
Today, St John Scotland’s Patient Transport Service provides free, comfortable and reliable transport to patients across the country. St John Scotland works closely with NHS Boards and the Scottish Ambulance Service to support patients who are being treated for cancer or receiving renal dialysis. These reliable services are coordinated and delivered by local Area volunteer teams. Following Angus and Dundee, further services were established in Fife (2017), Central (2020) and Edinburgh (2022). St John Scotland continues to work to expand Patient Transport services to new parts of Scotland, with valuable input from existing volunteers.
To learn more about St John Scotland Patient Transport, see:
www.stjohnscotland.org.uk/home/patient-transport
Patient Transport has been a passion of many St John Scotland members and volunteers for nearly twenty-five years, and several of them shared their memories with us.
John Calvert was a very pro-active person and Stranraer is very geographically isolated, so I think, at that time, and I think it is still the case, people that required cancer treatment, in essence, have to go to the Western General in Edinburgh and, as I understand it, NHS Dumfries and Galloway have a contract with NHS Lothian for treatment. The problem was, yes, turn up at the hospital in Dumfries and we’ll get you to Edinburgh. How do people get from Stranraer, the western end of the region, to Dumfries? That was something that was picked up by John Calvert, so that’s where the transport service started and apparently, it’s been an absolute godsend and it’s been appreciated by so many people, and I don’t know how some people get on without it. It’s not exclusively to Dumfries, sometimes maybe people go to Carlisle for treatment. There’s been quite a bit of rumble in the local press about why go to Edinburgh when, nine times out of ten, on the buses leaving from Stranraer, you’re going through Glasgow on a motorway to the big cancer centre in the west end of Glasgow, and there’s been quite a lot of local opinion on driving past Glasgow to go to Edinburgh, ‘So why can’t we go to Glasgow’. So, people go to Glasgow, people go to Crosshouse in Kilmarnock, they get some treatment there, and on one occasion it was an exceptional thing, but somebody panicked and I’m not sure about the treatment but it was very cancer-orientated, and two of our guys took somebody to Aberdeen and back. It wasn’t Christmas Eve, but more or less that sort of time, but it just shows the volunteers, the type of people we have, that if someone needs help, let’s do what we can.

Willie Waterson [pictured below on the right] is now the Patient Transport Coordinator in the West Galloway Area and explains his role:
[When I started as a driver] the role involved them phoning up and asking if I’d be able to drive to Glasgow, Edinburgh, on so and so a date, and I’d say, ‘Aye, no bother’. So, I just phoned the hospital, go into A & E to collect the keys, and on you go. When you come back, you fuel up and put the keys back into the hospital. It’s only transport of cancer patients we do; some are going for treatments; some are going for consulting; it’s different categories, but they are all cancer patients in different levels. It’s good to know I’ve done something to help someone that’s going through this terrible, terrible, time of their life. That’s the way I look at it.
I’m still a driver and became Coordinator about seven years ago… The Coordinator duties is just organising the transport. I’ve got the phone here and it’s just for St John’s, it’s not personal to me; it’s paid for by St John’s and the number of this phone. The college’s secretary uses [the number], the drop-in centre in Stranraer, doctors’ surgeries and patients use it. As long as it’s cancer related, we’ll do what we can for them. That’s the way it was set up in the Stranraer and Wigtown area by the late Dr John Calvert, and how it was to get to these hospitals when they have no other means of getting transport and that’s why it’s open to all cancer patients in this area. So I note the dates in the diary, contact the patients and when I’ve got a driver, I phone and say a driver will pick you up at the hospital or at home at so and so a time, and they’ll take you, and the driver’s name is so and so, and I pass the patient’s name and a contact number on to the driver so the driver knows who they are, where they are going, and away they go. The driver takes them up, makes sure they get to the right department where they are going at whatever hospital and brings them back home. If I couldn’t get hold of a driver, I would go myself but there’s always a driver because they’re a good bunch.
I was approached by a couple of people from Headquarters in 2016 because I used to work in Fife in the Health Board; they were wanting to set up patient transport within Fife and they thought I would have some contacts. So basically, I went to a couple of people that I knew, and they pointed me in the right direction to the people to get it sorted out. We had a meeting with the dialysis people, and they said, ‘How soon can you start?’, basically, because otherwise they would have to rely on the ambulances and sometimes they are rather draughty, so the patients would much rather be in cars if they could. We only take patients who can walk themselves; anybody else, the Ambulance Service has to cope with that, because our people are just drivers, they’re not trained in patient handling. Basically, we have a pool of about twenty odd drivers, and we started off at Queen Margaret Hospital because it was a smaller unit than Kirkcaldy, and then after a year, it was so successful that Kirkcaldy wanted us to start off there as well. So, we now run a service with both units.
The drivers of the first shift in start about six o’clock in the morning because the patients have to be in by seven, so the drivers have to pick up the car, check it, make sure it’s alright and then go and pick up the first patients and have them in for seven o’clock. With Covid, it’s been a bit more difficult because it’s been one patient in a car at a time, whereas before we could take up to four, so the drivers have a wee bit of a longer day just now. The drivers who come in for the lunchtime shift, they bring in the afternoon patients and take the morning patients home and the evening shift comes in about five o’clock and they bring in the evening patients and take the afternoon patients home. We do this five days a week at both hospitals.
I was thinking, ‘What am I going to do when I retire?’, and Mary [Bill’s wife] having had her stint of breast cancer, we were at the doctors and saw the flyer just saying, ‘Drivers Required’ to transport patients to the hospital. And after having the flyer for two years, I picked up the telephone, dialled the number, and I made contact with someone who I admired one hundred per cent. His name was Bill Spence. He’s no longer with us; he died just about 18 months ago, but Bill sort of took me through everything that he expected of drivers, and how he wanted St John Patient Transport to be the best, not just as good as, it had to be the best. You know, you were treating the patient, giving them that extra bit of comfort while they were on their way. Initially I was taking patients to the Cancer Unit in Dundee, and the first patient I had was an old lady of 84 and she was fearful of going for this first piece of treatment, and I said, ‘Oh my wife’s been through it’, and she immediately told me all about it. Eventually, she was like an old friend. Every time I turned up to take her to hospital she said, ‘Oh, you’re here’, that sort of thing. I took her in [the clinic]; the treatment only lasts about ten minutes; she lived about ten minutes from the hospital, so you’d ten minutes in the car with her, took her in and she got her treatment for ten minutes so you were only waiting for ten minutes, so that was the shortest I ever had. And I had one which was outside Blairgowrie, and that was about thirty-eight miles, and so you were taking them in, they’ve still got the ten-minute treatment, and it was 30-45 minutes to take them back again.

We’re a bit late to the party here but we are up and running now. Other areas in St John have been doing this for decades. We thought we would start and then the pandemic came and then we realised we’re going to have to start this during the pandemic and it has been done. So yes, in Edinburgh we are very proud to be offering volunteer Patient Transport to renal patients at the Royal Infirmary. We are just coming out of the pilot phase at the moment but we hope to be offering more opportunities for more volunteers and providing a regular transport service for more people who require just that little bit more assistance to get to their dialysis appointments.
As you can imagine there’s lots of contracts you have to go through, so you have to wade through that with the local health board. The day to day is dealt with by NHS staff who run the unit on the ground, developing and maintaining relationships there. They understand the value a volunteer patient transport driver can bring to their patients and so we have a couple of coordinators who assign people to patients and patient journeys and they work very closely with the unit administrator who oversees who’s coming in and at what time.

Ian Clarke and Carol Campbell are drivers in the West Galloway Area.
Here, they recall how they got started and their first experiences.

I’d been up here about three years [from Yorkshire] and I was talking to a chap, Adam, who used to be one of the organisers for the transport. I was talking to him and he said, ‘Do you like driving’, and I said, ‘Yes, all my life I’ve done driving’, and he asked me to go with him to Glasgow, to Gartnavel Hospital. He told me about the organisation, so I went with him and we had a client, so he asked me if I’d like to be a driver. So, I started, and it’s about 12 years I’ve been driving for them. I thoroughly enjoy it. I enjoy talking to people. Having had the problems that a lot of people I take up have had, I can relate to them, talk to them, put them at ease about what they’re going to go through when they get to the hospital, with the radium treatment and that sort of stuff, because I’ve been through it. I am fine, I am one hundred per cent… I think having been through treatment, it does help; you can relate to them and relieve their anxieties more. The first operation I had, I was told if I had left it a fortnight, they wouldn’t have been able to do anything for me; it was that close because the type of cancer I had was doubling in size in 24 hours. So, I was seen by the doctor on the Friday, I was in hospital on the Sunday, and operated on the Monday. It was as quick as that, but that was in Yorkshire and I’ve had it in my neck since I’ve been up here, and touch wood, I’m fine, a check-up every three months. So yes, I believe you can talk to people, you know what their fears are, especially if it’s their first time going up to have treatment. So, it’s easier to talk to people and put them at ease.
I think it’s a good service, it’s a great service, and I know with the few I have done, they are all very appreciative of it, and that’s good, isn’t it? I mean, it’s terrible if you are sitting at home worrying about how you’re going to get to hospital. I stopped at the bus stop one day in Dumfries, a man was waiting for the Stranraer bus and I was doing some shopping, and he said, ‘Oh this awful. I had to come up this morning and I had to get out from the hospital to here, and then I have to get back to Stranraer.’ And this was before I knew about St John’s, and I thought, it is awful. It is awful. I thought that man should’ve been offered help by his GP or his consultant. That’s really my view on it. I think, make it more available, if possible. Everybody has constraints on what they can do, and Willie [Waterson] explained when they bought the second car, it was because they were so busy.
It’s a great service that St John offer and I’m really quite proud to be part of it. It’s something that’s lacking. I mean, [this area] is a long way to any of the major hospitals and there are people who probably wouldn’t know which way to turn to get there. So, I think it’s great, and when Willie explained it to me, he was very open and honest and welcoming, and he seems to do a really good job.
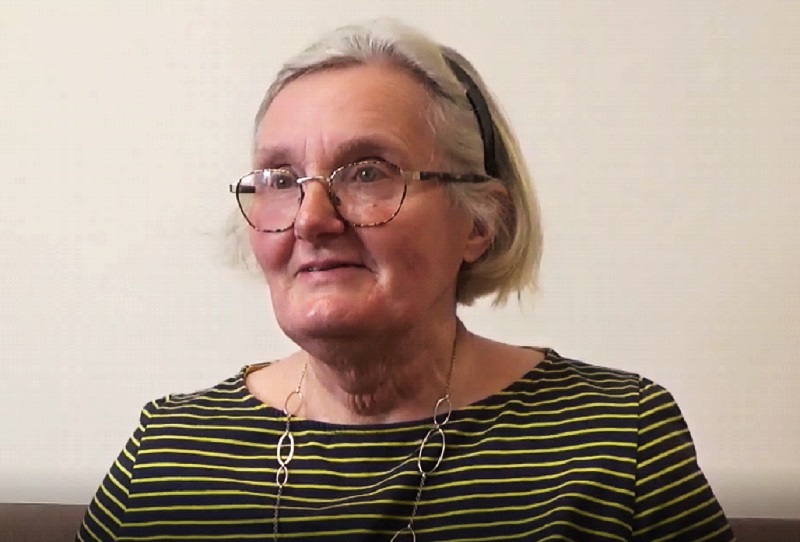
It’s the best thing [a volunteer] could do, it really is the best thing they could do. They’d get a lot out of it, a lot of benefit out of it themselves, meeting people and understanding some of their problems, and feeling that you’ve done something worthwhile to help somebody. It’s a joy. So, anybody that can drive and can drive safely and properly, it’s the biggest worthwhile cause, the biggest charity that’s going, and they can help; they’ll see something at the end of it.
Patients are indeed appreciative, as illustrated by this letter from a patient in West Galloway:
Dear Liz,
I’d like to take this opportunity to thank the fantastic St John Transport Team. When I was diagnosed in March this year (that is in 2021) one of the major concerns my wife and I had was how we were going to get back and forth from Hospital appointments. I was unable to drive and my wife does not drive. Most family and friends are working. A friend suggested we contact St John’s that they might be able to help. We contacted Willie. After a five-minute conversation he assured us that he and his team would look after us, this really did take a great weight off our shoulders. I have to give a special mention to the drivers, nothing was too much trouble. If I was a bit late coming out of Hospital it did not matter as long as I was comfortable, they took their time and got me home. They could sense when I wanted to talk or when you wanted a quiet time, a rare gift indeed. I will always be thankful to St John’s Team as they give up so much of their time to help others. Long may they continue with this fantastic work, they give so much to our community.
Best Regards
Diana Orr Ewing was one of the recent patients to receive assistance from the West Galloway team:
I think I was just told about it because I ended up requiring to go to Edinburgh for therapy in the winter and it wasn’t feasible to have driven up every time and so I asked around… This was in March this year… [The service] was absolutely wonderful. They came and met me, collected me at home, collected my bags. They were really good on the journey, you didn’t have to chat all the time, they had great empathy to know when you were ready to have a chat or when you weren’t. And they delivered me in Edinburgh and picked me up at the end of my month’s treatment and brought me home.
I’d just like to say how very grateful we are and I shall be telling everybody about the wonderful service in Stranraer, and I will pass the word far and wide. I think anybody who needs hospital transport should always remember St John Scotland.
CPR TRAINING
In 2015, Scotland’s survival rates for cardiac arrest lagged far behind those of other European countries, at only 5%. In response, the Scottish Government brought together emergency services, charities and community groups to tackle the issue, and set out the target to save an extra 1,000 lives by 2020. St John Scotland joined this partnership – known as ‘Save a Life for Scotland’, to help strengthen the fight to save lives from cardiac arrest.
By 2019, CPR training was an important focus for St John Scotland and across the country, St John Scotland volunteers were working hard to spread knowledge and awareness in their communities. They knew that this was making a difference as the then latest statistics revealed that bystander CPR had increased more than 20% in the previous five years, and as a result, survival rates from cardiac arrest had doubled.
Improving public awareness was paramount as quick action is vital to saving lives. Most cardiac arrests happen in the home, with many more occurring in people’s workplaces, or out and about in the community. That means that it is members of the public, rather than medical professionals or paramedics, who are often needed to act first and start CPR before the ambulance arrives. For every minute that passes without action, the person’s chances of survival decrease by 10%. To give someone the best chance of surviving, it is important that someone nearby understands what has happened, knows what to do, and has the confidence and skills to take appropriate action.
Across the country, St John Scotland volunteers have taken and continue to take this message into their local communities. From shopping centres to summer fairs, community drop-ins to youth group meetings, local teams of St John Scotland volunteers provide free training to groups, and each year they have helped thousands more people learn the skills to save a life.
To learn more about St John Scotland CPR Training, see: www.stjohnscotland.org.uk/home/cpr-training
One of the things that we have become immersed in over the last few years is the CPR training, and the husband-and-wife team, [Malcolm MacBean and Jane MacBean], they travel extensively to do CPR training, and whilst they are there, they have encouraged new trainers to join, which they have done. We have a young volunteer in Wick, who does the CPR training. We also have one in Skye.
We also have a demonstration defibrillator and will show people how to use them as well, but some people are scared of them, they think they’re going to electrocute themselves or the patient, although electrocuting the patient is the object of the exercise. So they think they’re actually going to hurt the patient, so we have a demonstration defibrillator that we can show people how easy it is. The machine talks to the people and tells them exactly what to do… if the machine detects a heartbeat, it won’t allow you to shock the patient, so they are fool proof.

Anne Mitchell (pictured below right) teaches CPR to a volunteer

When I first retired, I was looking for what I could do to fill in my time, I had been a very active person, I was still working full time, not so much nights but did on-call at nights. I was used to being active and ‘Save a Life Scotland’ was advertising quite widely at that point, and I contacted them and was put in touch with St John and I’ve been with them ever since. I’ve gone from being a CPR champion to a CPR Lead for the ‘St John in the City Defibrillator Project’ in Edinburgh.
The actual sessions are relatively short. You have to assess, particularly with Covid, you have to assess where you are going to be teaching in, but it varies hugely. You could be doing a primary school with Primary 7 and working your way down [the school years], and what you teach is very different from Primary 1, with a teddy bear and “Do you know where you live?” [if you have to call emergency services], to the Primary 7s who want to know how to do [CPR] but they may not have the strength, but they could show an adult what to do. Your language and body language is very different to an older group, perhaps in sheltered housing, again, who for fragility reasons might not actually be able to do the process, but they can understand it and they can tell that person who’s passing by and would like to help but doesn’t know what to do, how to do it.
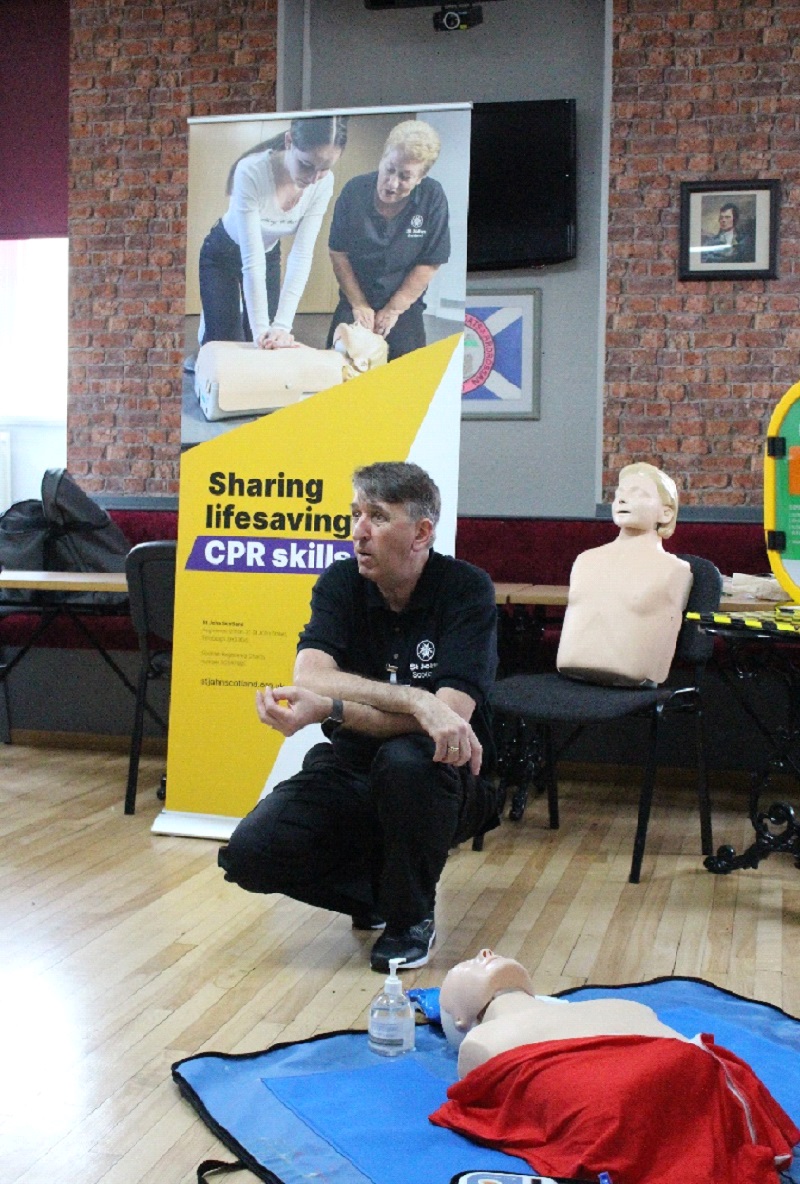
I previously heard about St John’s Ambulance, I was under the illusion that St John Scotland was under the same branch, but one of my close friends said to me that St John Scotland is a totally different organisation in Scotland, taking to do with CPR and defibrillator training, and with that going through, he asked me if I would be interested in volunteering, because he knew my background to do with first aid and training. And I said, “Yes, certainly I’ll come along.” That was on the 27th of November last year [2021]. I dooked my toe in the water, shall we say, and it’s taken leaps and bounds from then, and I have now taken on the role of CPR Lead Champion in Ayrshire and Arran.
My role in St John Ayrshire and Arran is basically training volunteers to do CPR and defibrillators. We call them CPR and Defib Champions. My role is basically to train them up to a standard that they can go out and train the public. I am already a hands-on kind of person so I actually go along with them to every training session. I conduct the training, and then I get them up to a standard that I am happy that they can deliver that training. Now, when that’s done, we, in private, without the public being there, give them [volunteer trainee trainers] practice on the defib, and give them practice on the manikins. Predominately, I am there to try and train them and give them the support and any help they need, and build confidence, so that they can deal with the general public and answer any questions that’s asked.
So, there are very different groups, and drop-in sessions. We did Port Edgar Open Day with the Water Centre down in South Queensferry, and we had 365 people all pass through our hands, all having a go on a manikin, but it was a beautiful sunny day so our problem there was not hypothermia, it was sunburn! So, it’s just trying to pre-empt what you’re going to need on the days, how many volunteers you’re going to need to carry out this training, whether it’s one, two or six people that’s needed and therefore how many manikins you need and spacing out now particularly post Covid and thinking about the safety of the volunteers as well as the people who attend… [The] challenges are getting volunteers that are available through the day because businesses want CPR taught through the day, Monday to Friday. Unless I’m using retired people like myself, then there’s not a lot of us available.
One of our volunteers was a young boy who volunteered to come and do CPR and Defib training, and he came along to a couple of sessions. He was very good. I saw the potential in him. I asked him would he be interested in talking to the school he was at. He was a sixth former. He spoke to the Deputy Head. The Deputy Head was really interested in it. So, what we did was ask Callum [the school student] if he would be interested in organising that. He organised it and it happened on Tuesday 19th April. We had twenty sixth formers who turned up to do CPR and Defib training, and that was just out of one boy who showed an interest. It was a really good day, actually. That boy has now gone on to be one of our volunteers, and he’s keen as mustard to come along to every session we’ve got.


Now we’ve started doing CPR as well at the same time, we teach people to do CPR. We’ve been to the Bon Accord Centre a few times and taught people to do CPR. The amount of people in Aberdeen who know it is unbelievable. We also go to two secondary schools and teach them to do CPR as well, one is quite good now, they can teach their own kids.
PUBLIC ACCESS DEFIBRILLATORS
A defibrillator can save the life of someone whose heart has stopped beating normally (‘cardiac arrest’) by re-starting it with a controlled electric shock. Modern defibrillators are portable and easy to use, and those used as Public Access Defibrillators are designed to be used by a person with no previous training; they give visible and audible instructions and will only administer an electric shock if required.
In 2006, Angus and Dundee Area Committee paved the way for a new St John Scotland project – providing defibrillators to local organisations. Tayside Police and Carnoustie Health Centre were keen to receive the machines, which cost around £1,200 each. Two were purchased at the end of the year. Angus and Dundee were to trial the project in the hope that it would prove successful and be rolled out to other areas and then extended nationally.
The following year, 2007, St John Scotland’s West Lothian committee allocated money to purchase two defibrillators, one for a local health centre and the other for a shopping centre.
In 2010, St John Scotland announced that it would develop work nationally to provide defibrillators for use in the community. Since then, they have worked with the public and several businesses and organisations, including golf clubs, Network Rail, community councils and others, to place lifesaving “heart-start” equipment across Scotland. In August of 2016, St John Scotland's Edinburgh committee launched the St John and the City public access defibrillator project at a Civic Reception in the City Chambers.
A further ninety Public Access Defibrillators were installed across the country in 2019, sited in prominent locations, including main streets, schools, gyms, scout halls, riding schools, and churches. Communities both rural and urban have benefited from access to the equipment.
Today, St John Scotland’s support for Public Access Defibrillators is through their Community Defibrillator Scheme, whereby community groups are offered part funding, advice and support to install the equipment. This is then followed up with free volunteer-led community training to help raise awareness, teach locals bystander CPR, and demonstrate how easy defibrillators are to use
Learn more about St John Scotland’s work in Public Access Defibrillators at: www.stjohnscotland.org.uk/home/defibrillators
St John Scotland volunteers Lynn Cleal and Andrew Smith talked about how they started the St John and the City Project in Edinburgh:

Now, Lynn and I moved from Edinburgh to Cove [on the Rosneath Peninsula] seven years ago. On the drive from Edinburgh to Cove we realised that we were passing through all these villages, and in the villages, we saw telephone boxes, and instead of the word ‘Telephone’ at the top, it had ‘Defibrillator’. We saw these boxes on the sides of community halls and you think, ‘Defibrillator, defibrillator, defibrillator.’ So, we got thinking about Edinburgh – urban area, large amounts of footfall, lots of tourists, and to us we just simply couldn’t see the boxes on the walls. And so spurred by the use of the defibrillators at Waverley Station and realising that there are plenty of big businesses, as well as individuals in Edinburgh, who are wanting to help, and they think the defibrillator is a good idea. We need to find a way to make it simple for them to provide funds to put defibrillators up, and where we thought we, as St John, could add value, is sorting all that out for them. You might have a large company wanting to say, “Well here’s enough money for ten defibrillators”, that’s great, but they don’t know where to put them, how to order them, all that sort of thing; and we figured it all out. We found the walls to hang them on, we found guardians to take care of them, so if their act was simply that of a financial donation, we can turn round and say to them, “We can put that money to good use - that by providing so many defibrillators, so many cabinets, we’ll get them up, we’ll provide a plaque with your name on it.”
That was how we’ve gone from that initial helping Waverley Station, the charity helping them by providing two defibrillators, and they provided two of their own, and it’s kind of mushroomed now, half a dozen years later, to having over 325 public access defibs in and across Edinburgh.

I engaged with the Lord Provost of Edinburgh at the time and he gave permission to have a civic reception, twice in fact, two different Lord Provosts, and on the back of that we got quite a lot of advertising. The problem we have with St John Scotland is, the majority of people think we are St John Ambulance, and it was really hard to educate people and to get them familiar with the brand in Scotland. So, the publicity was quite a big thing for me, so people could see it, and from the civic reception it ended up - it grew arms and legs. Obviously, everybody knew about it, so the airport wanted defibrillators, and the police stations wanted defibrillators, so I said to the Lord Provost, ‘Why don’t we look at the trams?’. And they’d had really bad press with digging up the roads, and I thought it would be a great way to give back, so they could show what they were doing. So, they agreed to put a defibrillator in every tram. So, we got thirty donors, and we installed them on the trams. So really, you’ve got a defibrillator passing every three minutes either side and they have been used several times. And the idea was, if there was an emergency anybody at the tram stop could push the emergency button and the next tram would come and stop with the defibrillator, and the call handler at the trams would notify the Ambulance Service, so that they would make it. Some of the tram stops are in awkward positions and it would be a case that they would make room for the ambulance to come up. So, it works. It’s a great team, and often where we’d had defibrillators, the tram would put a spare set of pads on to one of their moving trams so one of my volunteers could get them and replace the pads.
It worked out perfectly for us and on the back of that, which is really excellent, is the trams now allow us to stand through the International Rugby stand at Murrayfield can collecting and usually after two or three sessions of can collecting at Murrayfield, we have enough money and we purchase a defibrillator and a cabinet. So, I think we’ve got five now, that the volunteers have fundraised off the back of the defibrillators and can collecting.

The idea was to try and take the fear out of everything to do with the defibrillators and make it easy, you know, because I’m sure the adrenaline must be pumping if somebody’s running to get the defibrillator. So, what we did was, we created this plaque, and it’s got ‘St John and the City Defibrillator Project’, and it has who it’s donated by, and underneath it’s got an emergency reference. So, if you were phoning 999 you would quote the reference, and I’ve already uploaded all the information on to the Circuit, which is the national database for defibrillators, and with that code they can then say, “We know you’re at EH6. The ambulance is on its way”, and it allows the person to take the defibrillator and go; they don’t have to worry about where they are, and I’m sure, myself, if there was an emergency, I wouldn’t know what part of town I was in, let alone your international community that we have, and the tourist business in Edinburgh. So we try to make it as easy as possible and the beauty of that, too, is that as soon as it has come off the database, that it’s away to be used, they then send me an email to say the defibrillator is being used in an emergency, so I know then to call upon one my volunteers, or myself if I’m in town, to have a spare set of pads to replace it, so it’s then put back in the cabinet ready for the next emergency. We’ve two or three that’s been out through lockdown; the Scott Monument one has already been out the cabinet six times over the last year or so, and the idea is to make sure that as soon as it goes back into the cabinet, it’s in working order and we’ve got all the information back on to the Circuit so it’s ready for the next emergency. The Scottish Ambulance and myself started to organise this about five years ago, and then the Circuit came on board. So, all of that information has gone over to them and the programme, as far as I’m concerned, is working really well, apart from when I get pinged at two o’clock in the morning to say the defibrillator is now out of the cabinet; so, I just send a quick email to somebody to check it the next day. So, it’s very good, it’s working well. It’s a great project.
Outwith Edinburgh, community defibrillators are also a priority:
We’ve just had the Prior hand over a defibrillator to the National Trust for Scotland, at Hill House in Helensburgh, the Rennie Mackintosh House. We are doing defibrillator training; we’ve been doing it through youth groups and churches. So, we’re developing that training and the supply of defibrillators where necessary… There are other charitable groups who are doing defibrillators, it’s become a popular thing, so we don’t really want to be trying to steal anybody else’s thunder. It’s just where there are gaps, we will fill the gaps if we can.

We also can provide defibrillators if we hear of places that need them. We have done it in Stranraer, and we did it at Newton Stewart Golf Club; we gave them a defibrillator there, and we don’t ask for any donation. The only thing we do ask is that once it is handed over, they register it with the Ambulance Service and they have the upkeep of it.
The defibrillators came first but the CPR was very, very close on its tail. From the word go, it was always a case if you’ve got a defibrillator, either the donor or the host, we would provide them with bystander CPR training. If you can imagine you are the owner of a business and you’ve got this yellow box on your wall, and you’re kind of wondering about what it is and what it does, and you might be a bit anxious about opening that door, then we have, since the beginning, provided that bystander CPR training, to help demystify it; to help reassure people these are automated defibrillators, they’ll talk you through it and under what circumstances you would do CPR, and how the defibrillator provides the icing on the cake in those circumstances. Yes, it’s a piece of kit, it’s a very clever piece of kit, but it’s not one that you need to be afraid of, and, just giving people that reassurance… We pitch up at local fayres, at libraries, community centres, people who ask. However, we have got a bit of a backlog at the moment because of the pandemic and we’ve continued to roll defibrillators out, so our CPR volunteers have got a very busy 2022, and probably into 2023, playing catch-up with who’s asked for bystander CPR training.
COMMUNITY FIRST RESPONDERS
Throughout 2011, St John Scotland conducted a National Project Review, headed by Bill Spence, Chair of St John Scotland’s Angus and Dundee committee. The review explored additional areas of need, identifying possibilities for cooperation, whilst avoiding duplication.
Bill’s initial report suggested two promising contenders as new national projects - an expanded patient transport service, building on existing provision, and ‘First Responders’, essentially providing rapid assistance to a person in suspected cardiac arrest before an ambulance arrives. Both these projects had been considered whilst keeping in mind the longstanding agreement between St John Scotland and the St Andrew’s Ambulance Association, which was intended to avoid unhelpful duplication and competition between the two charities. Following discussions between the two organisations, St Andrew’s open-mindedly agreed that the demand for patient transport and first responders was so great that there was plenty of room for multiple providers for the foreseeable future. As St Andrew’s raised no objections to St John Scotland pursuing these programmes, the latter began preparations.
Under his leadership, in 2012, Bill Spence introduced a pilot First Responder Scheme in Angus and Dundee. First Responders are members of the public who volunteer to help their community by responding to medical emergencies while an ambulance is on its way. They are trained in a range of emergency skills, including CPR (cardiopulmonary resuscitation) and the use of defibrillators and oxygen masks. A First Responder is then able to provide an early intervention in situations, such as a suspected cardiac arrest, if they are able to reach the scene before the ambulance crew can get there. This can save the life of a patient or increase the chances of them making a full recovery. Volunteers are deployed by the Scottish Ambulance Service in response to an emergency call. They arrange to be on an on-call roster for specific periods, during which they have access to a defibrillator and other equipment.

Bill Spence working with Scottish Ambulance Service representative Murray McEwan on arrangements for the First Responder scheme
When a report of an incident is received by the Scottish Ambulance Service, they dispatch a paramedic crew, but where a First Responder is also available locally, and the incident is within their level of competence, they will task that volunteer to attend. This may be as a lone responder or with a supporting trained ‘buddy’. They then apply their skills in resuscitation to a patient that has collapsed with suspected cardiac arrest or similar symptoms. On arrival of the Scottish Ambulance Service crew, the First Responder(s) hand over treatment to the paramedics and assist them in any task they are given, which could be to support relatives at the scene.
During that first year, around twenty St John Scotland volunteers received training, and responded to 202 calls. Volunteers must pass a proficiency test before being authorised to attend calls; they then receive continuity training to maintain their skills.
During the following years, and outwith Angus and Dundee, St John Area committees have supported existing local Community First Responder Teams with funding. In 2014, St John Scotland’s Highland committee funded two Cardiopulmonary Resuscitation (CPR) meters for the Point First Responders on the Isle of Lewis; the Ayrshire and Arran committee provided start-up funding to the Fenwick First Responders; in East Renfrewshire, the Glasgow committee supported the Neilston & Uplawmoor First Responders.
Learn more about St John Scotland Community First Responders at: www.stjohnscotland.org.uk/home/community-first-responders

William Harvey, known as Bill, explains how he got involved as a Community First Responder:
Two years after I joined as a [Patient Transport] driver, Bill [Spence] had another project which he was bringing online and he was looking for people in the area to be First Responders. People who would turn out when the 999 call came in, and the Ambulance Service would notify the First Responder closest to the patient, and you’d be there performing your duties, maybe half an hour before the ambulance arrived, or maybe longer. In the time I was First Responder for this area, I was out five times but I was on duty maybe one hundred times.
The training for that is first class. You are trained in CPR, and you’re trained in the use of the defibrillator… People would come along from the Ambulance Service and give a talk or a show, sort of thing; they would have different scenarios that they would put to you and you’d talk your way through them, say what happens. And if there’s a shout for an ambulance, and if there’s a defibrillator close by, and if the First Responder is needed, they’ll say, “That’s where your defibrillator is”, and within minutes you’ve got someone who can apply the defibrillator, if that’s necessary, because it’s the first 8-10 minutes that makes all the difference. If you can get there quickly and get the defibrillator on, there’s a 25% chance of saving a life.
Bill Spence organised the first defibrillator in our village hall. I think it has just snowballed; there must be close on 100 all over Angus and there’s a lot of private ones as well. People have a bereavement and they say, “I want to put £1,000 towards a defibrillator in the area”. I think Carnoustie has something like five on the High Street but the important thing is you want them to be available 24 hours a day. Some people have a defibrillator in their shop and when the shop is closed the defibrillator is not available. Those days of mouth to mouth are long gone; it’s CPR done the proper way. To see it being done on ‘Casualty’, on the telly, that bears no resemblance to shaving the chest and making sure the pads are gripping; and once you’ve pressed that button you’ve got to be clear because it gives a kick. It is an experience I’ll always be thankful for.